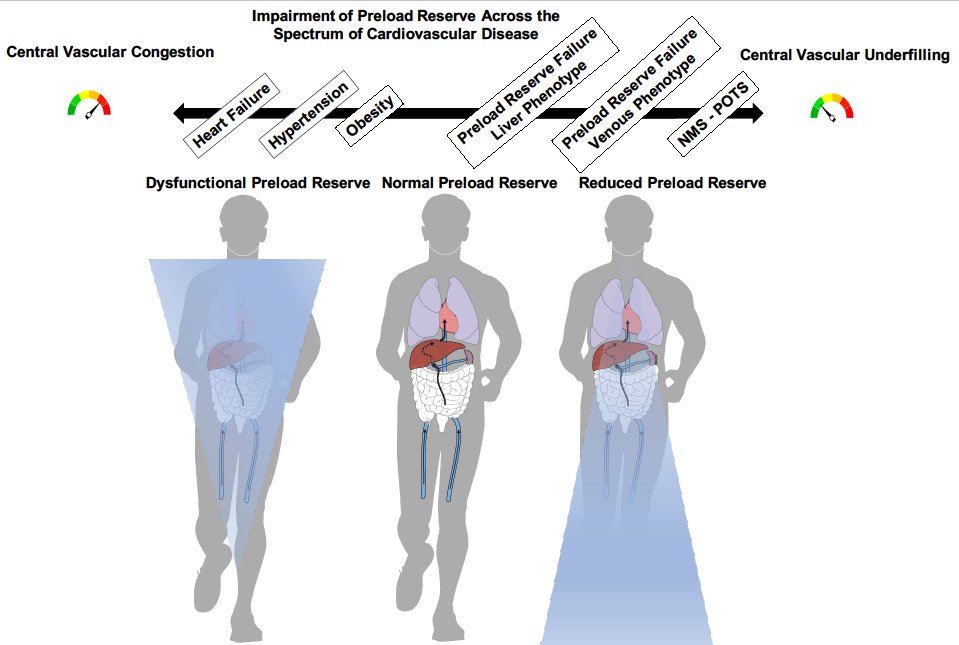
1. "Heart" Failure is not only a problem of the heart. The ability to modulate preload (aka Preload Reserve) is central to activity/exercise. Find the review on  Extracardiac Abnormalities of Preload Reserve in HFpEF
Extracardiac Abnormalities of Preload Reserve in HFpEF
@sobotka_paul MarkDunlap @CircHF
https://www.ahajournals.org/doi/full/10.1161/CIRCHEARTFAILURE.120.007308#.YAgC6YbM14k.twitter
 Extracardiac Abnormalities of Preload Reserve in HFpEF
Extracardiac Abnormalities of Preload Reserve in HFpEF
@sobotka_paul MarkDunlap @CircHF
https://www.ahajournals.org/doi/full/10.1161/CIRCHEARTFAILURE.120.007308#.YAgC6YbM14k.twitter
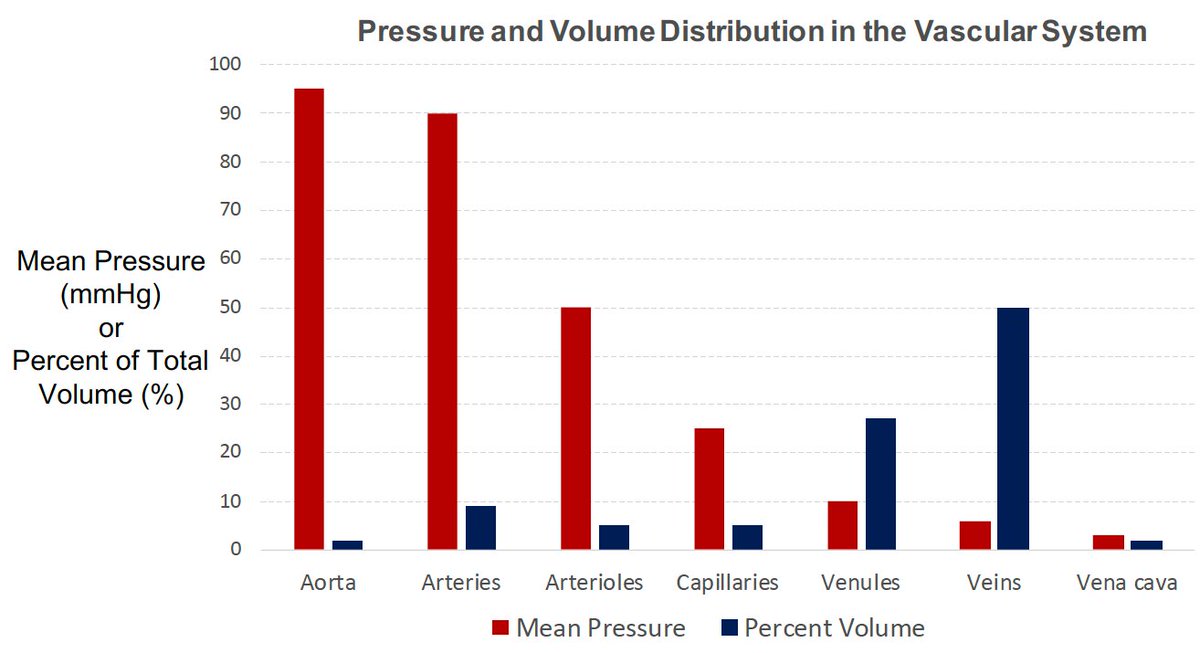
2. Majority of intravascular blood volume is located in the venous system. Veins are highly innervated (in many instances more so than arteries). The abdomen pools the majority of the blood volume and blood can be recruited quickly in and out of the compartment.
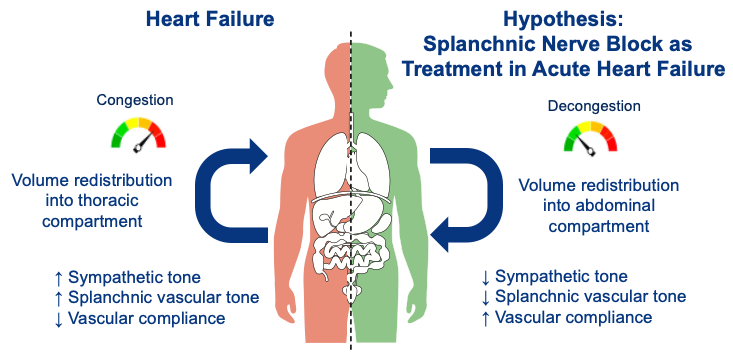
3. In heart failure chronic or acute loading of the heart with preload can in large parts explain the exercise induced elevations in filling pressures. A key source of blood volume is the abdomen.
https://pubmed.ncbi.nlm.nih.gov/8238596/
https://pubmed.ncbi.nlm.nih.gov/21934091/
https://pubmed.ncbi.nlm.nih.gov/28862947/
https://pubmed.ncbi.nlm.nih.gov/8238596/
https://pubmed.ncbi.nlm.nih.gov/21934091/
https://pubmed.ncbi.nlm.nih.gov/28862947/
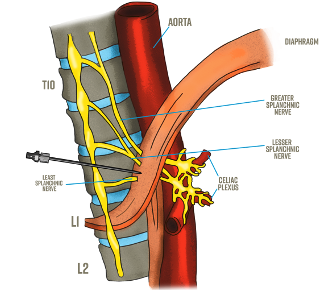
4. Could an inhibition of blood volume redistribution from the abdominal compartment improve exertional capacity in HFpEF? Studies testing splanchnic nerve blockade are exploring just that.
5. Yet, not only conditions with too much preload can cause symptoms of heart failure. Lack of preload augmentation with activity (preload reserve failure) will limit function. This is very likely to be mislabeled as heart failure with normal ejection fraction aka HFpEF
Lack of preload augmentation with activity (preload reserve failure) will limit function. This is very likely to be mislabeled as heart failure with normal ejection fraction aka HFpEF
 Lack of preload augmentation with activity (preload reserve failure) will limit function. This is very likely to be mislabeled as heart failure with normal ejection fraction aka HFpEF
Lack of preload augmentation with activity (preload reserve failure) will limit function. This is very likely to be mislabeled as heart failure with normal ejection fraction aka HFpEF
6. Conditions leading to preload reserve are:
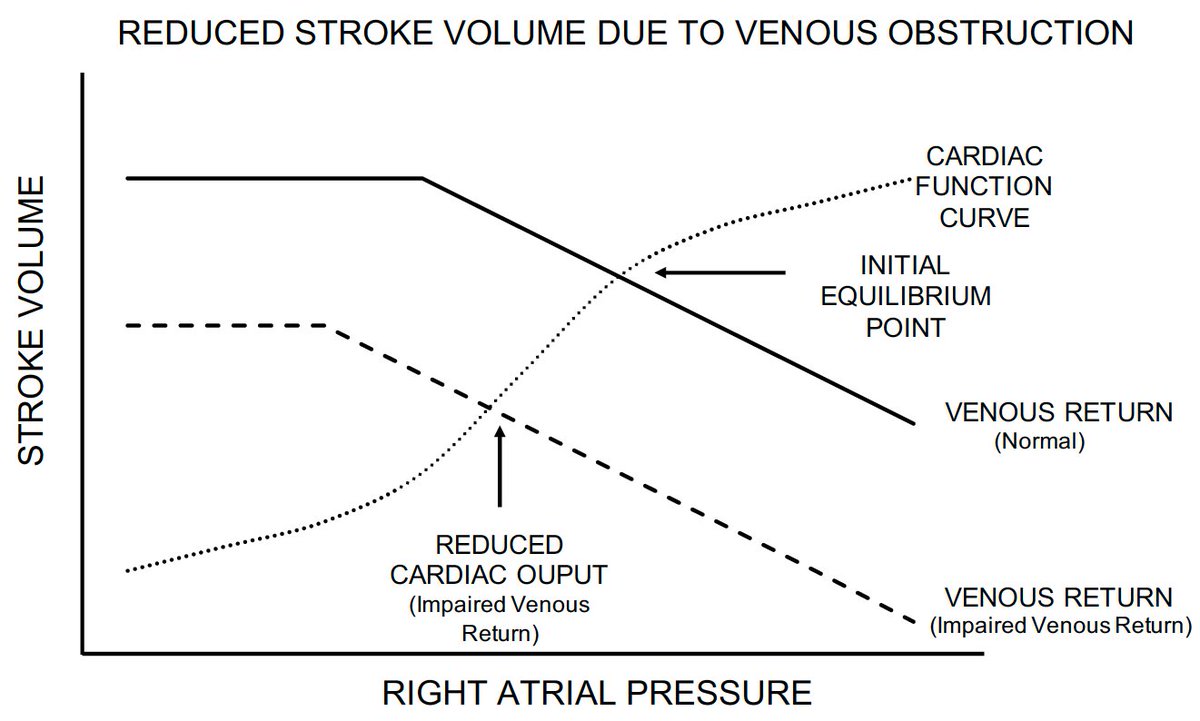
- Obstruction of Venous Return From the Lower
Extremities. Return of venous blood is impaired cardiac underfilling. Patients with venous obstruction have lower peak VO2. And resolution of venous obstruction improves peak VO2.
cardiac underfilling. Patients with venous obstruction have lower peak VO2. And resolution of venous obstruction improves peak VO2.
- Obstruction of Venous Return From the Lower
Extremities. Return of venous blood is impaired
 cardiac underfilling. Patients with venous obstruction have lower peak VO2. And resolution of venous obstruction improves peak VO2.
cardiac underfilling. Patients with venous obstruction have lower peak VO2. And resolution of venous obstruction improves peak VO2.
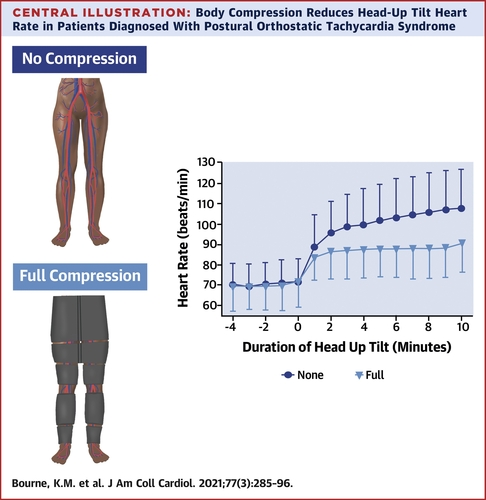
7. Autonomic dysregulation such as POTS, neurogenic orthostatic hypotension prevent cardiac filling with upright position, impair exercise function. Often the only therapy that works is "abdominal compression" increase preload.
increase preload.
https://www.thelancet.com/journals/lancet/article/PIIS0140-6736(97)24003-1/fulltext
https://www.jacc.org/doi/10.1016/j.jacc.2020.11.040
 increase preload.
increase preload. https://www.thelancet.com/journals/lancet/article/PIIS0140-6736(97)24003-1/fulltext
https://www.jacc.org/doi/10.1016/j.jacc.2020.11.040

 Read on Twitter
Read on Twitter