DNA test can quickly identify pneumonia in patients with severe COVID-19, aiding faster treatment. 1st authors @maesmailis @EllenHigginson Joana Pereira‐Dias
@JanineLux @jbartholdson @efkay88 @razmahroof @IslamAbdelaziz1 @GordonDougan1 @Baker_Lab_Cam
https://ccforum.biomedcentral.com/track/pdf/10.1186/s13054-021-03460-5.pdf
@JanineLux @jbartholdson @efkay88 @razmahroof @IslamAbdelaziz1 @GordonDougan1 @Baker_Lab_Cam
https://ccforum.biomedcentral.com/track/pdf/10.1186/s13054-021-03460-5.pdf
Press summary here - describing how we used a rapid diagnostic test developed by @CUH_NHS clinicians led by Dr Vilas Navapurkar, PHE scientists led by Dr Martin Curran and University of Cambridge scientists, to aid management of pneumonia. https://shar.es/aoCghs
To explain: Patients with COVID-19 who develop severe respiratory failure often need to be ventilated, and it takes a long time for their lungs to heal. They often remain on a ventilator for several weeks, sometimes months https://www.bbc.co.uk/news/uk-53217014
When patients are ventilated, their natural defences are bypassed and so pneumonia risk increases
https://en.wikipedia.org/wiki/Respiratory_tract_antimicrobial_defense_system
image from BJM 75 https://commons.wikimedia.org/w/index.php?curid=89265925
https://en.wikipedia.org/wiki/Respiratory_tract_antimicrobial_defense_system
image from BJM 75 https://commons.wikimedia.org/w/index.php?curid=89265925
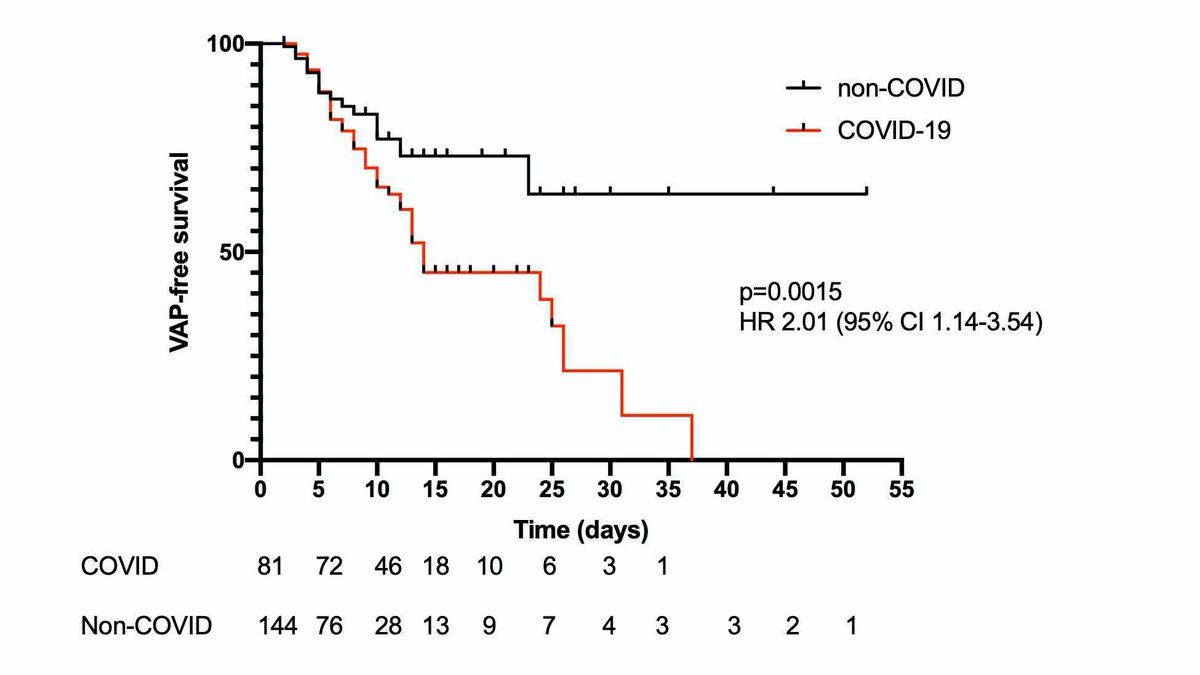
However, we found that it wasn’t just being on a ventilator for prolonged period of time, patients with COVID appeared to have increased risk independent of duration of ventilation
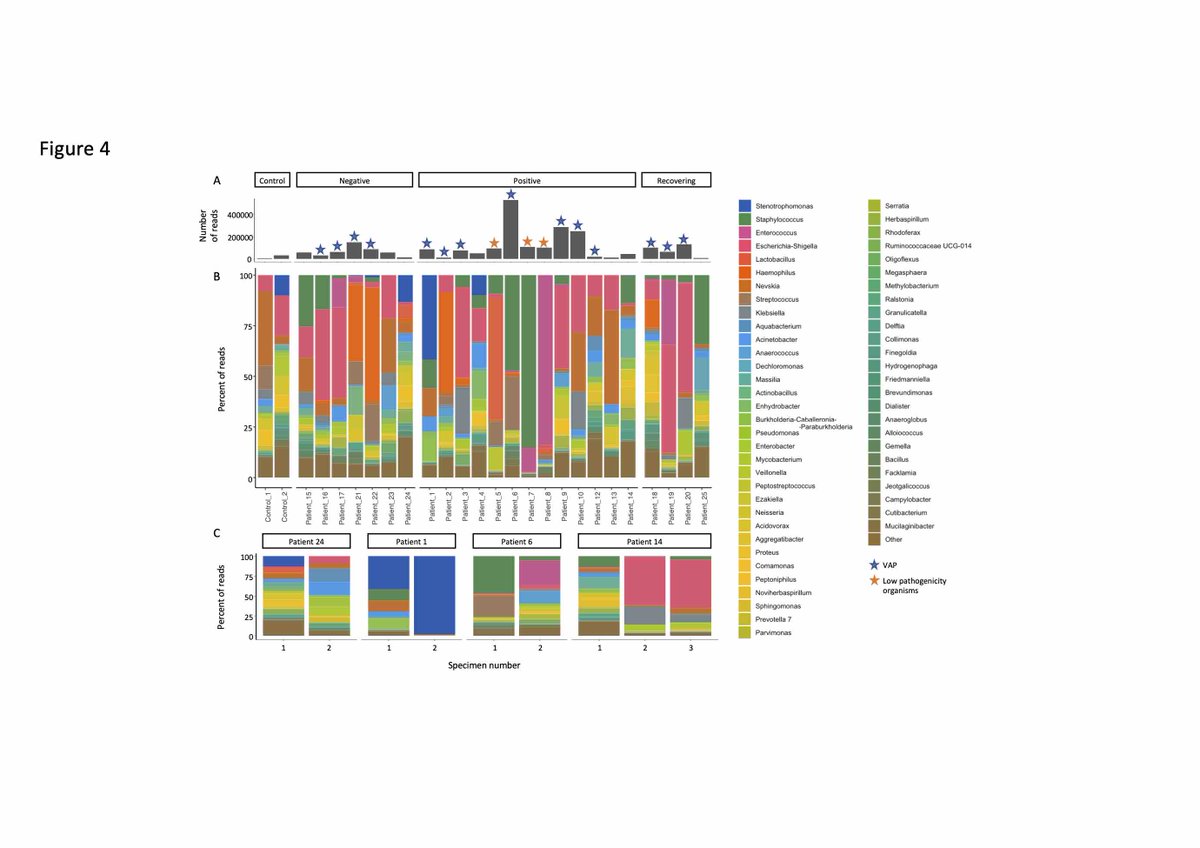
This wasn’t because the virus changed the microbiome of the lungs, as this looked pretty similar to what was seen in patients without COVID – and showed the effects well described in other groups of ventilated patients
We found that the bacteria that caused infection were similar to those which infect patients without COVID, but also there were increased rates of aspergillus (mould) infection and reactivation of herpes viruses.
Nephron, CC BY-SA 3.0 https://creativecommons.org/licenses/by-sa/3.0
Nephron, CC BY-SA 3.0 https://creativecommons.org/licenses/by-sa/3.0
This points to patients with COVID having impaired antimicrobial defences, which is no surprise as disordered immune function including impaired antimicrobial defences is often seen in sepsis - @msh_manu team reported this earlier this year https://www.nature.com/articles/s41591-020-1038-6
This study was facilitated by a 52-pathogen array that we have developed, and finished testing shortly before COVID hit. We were able to rapidly role this out in @CUH_NHS, innovating during a pandemic and shortening times to diagnosis and treatment https://www.medrxiv.org/content/10.1101/2020.06.02.20118489v3
What lessons do we draw from this? Look out for VAP in COVID, standard ICU antibiotic protocols apply, but be aware of mould infections such as aspergillus especially if the patient is not responding to antibiotics.
Thanks are due to the many people involved in this study, and the clinicians who developed and undertook the safe bronchoscopy approach used for diagnosis.

 Read on Twitter
Read on Twitter