The eGFR correction factor was introduced in the 90s on the basis that Black people have higher levels of creatinine than whites, though their kidney function seemed similar. 1/5
#healthequity #raceinmedicine #diagnosis @MClerkship https://www.nature.com/articles/d41586-020-03419-6#ref-CR2
#healthequity #raceinmedicine #diagnosis @MClerkship https://www.nature.com/articles/d41586-020-03419-6#ref-CR2
In the US, Black people are affected by kidney failure 4x as much as white people. It’s unclear how much the eGFR algorithm contributes to this epidemic, as systemic racism and socio-economic inequalities also play a big role. 2/5
Researchers argue that the eGFR correction actually makes the kidneys of Black people seem healthier than they are. Moreover, it promotes the idea that different races have different biology, blurring the enormous genetic diversity within racial groups. 3/5
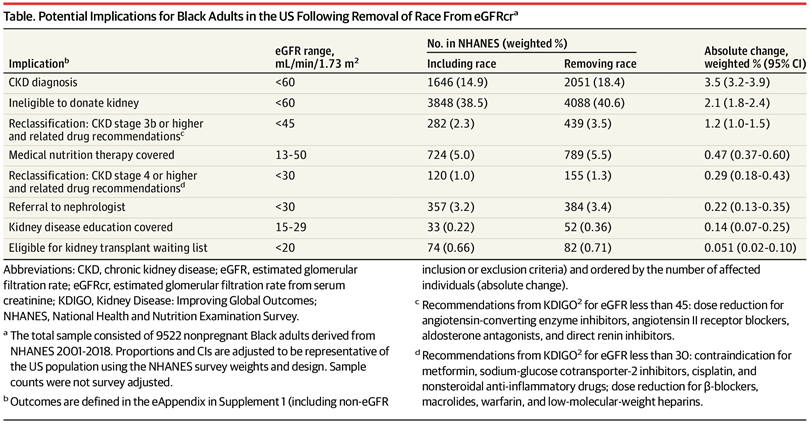
In JAMA, researchers assessed how removing the race-based correction factor impacts diagnosis. 3.5% more Blacks were diagnosed with early stage kidney disease, which would be 1 million Blacks in the US population. 4/5
On the flip side, access to common and affordable medications for hypertension or diabetes could be restricted due to kidney side effects. Instead of a race-based correction factor, revamping the algorithm to include other biomarkers beyond creatinine is a possible solution.

 Read on Twitter
Read on Twitter