1/12 A question that keeps popping up: what is the impact of #COVID_19 on global bacterial #AntimicrobialResistance rates?
-A thread with links to recent papers on this topic
(please add missing resources to this thread)
-A thread with links to recent papers on this topic
(please add missing resources to this thread)
2/12
Here are the links for the PRO-CON debate published in JAC-AMR:
PRO: "Disruptive direct and indirect effects of COVID-19 globally on economic systems, governance and public health expenditure and infrastructure may fuel AMR spread. " @ClancyNeil https://academic.oup.com/jacamr/article/2/3/dlaa049/5872561
Here are the links for the PRO-CON debate published in JAC-AMR:
PRO: "Disruptive direct and indirect effects of COVID-19 globally on economic systems, governance and public health expenditure and infrastructure may fuel AMR spread. " @ClancyNeil https://academic.oup.com/jacamr/article/2/3/dlaa049/5872561
3/12
CON:
"For this debate we show why, overall, COVID-19 will not result in increased AMR prevalence. But globally, changes in AMR rates will not be uniform." @CollignonPeter
https://academic.oup.com/jacamr/article/2/3/dlaa051/5872562
CON:
"For this debate we show why, overall, COVID-19 will not result in increased AMR prevalence. But globally, changes in AMR rates will not be uniform." @CollignonPeter
https://academic.oup.com/jacamr/article/2/3/dlaa051/5872562
4/12 Recent paper by @ClancyNeil in Clinical Infectious Diseases @IDSAInfo addresses AMR rates in bacterial superinfections.
"Stewardship will have a crucial role in limiting unnecessary antimicrobial use and AMR." https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7197597/
"Stewardship will have a crucial role in limiting unnecessary antimicrobial use and AMR." https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7197597/
5/12
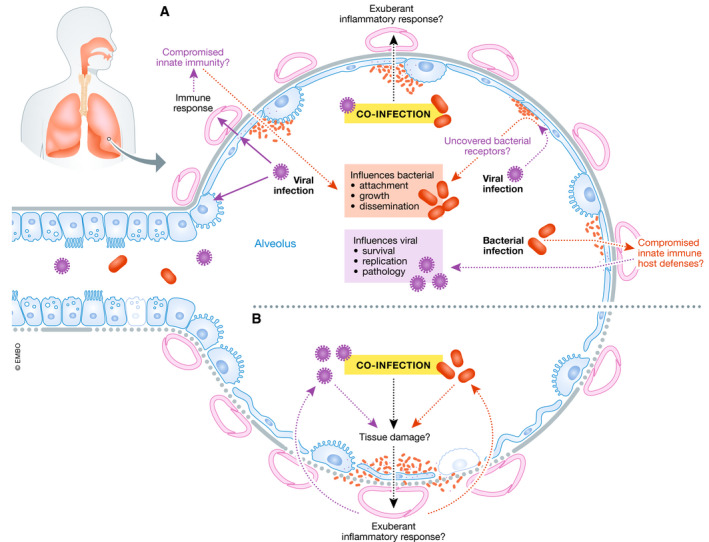
A viewpoint on "SARS‐CoV‐2, bacterial co‐infections, and AMR: the deadly trio in COVID‐19?" in @EmboMolMed by Dr. Bengoechea and @cggbamford
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7283846/
A viewpoint on "SARS‐CoV‐2, bacterial co‐infections, and AMR: the deadly trio in COVID‐19?" in @EmboMolMed by Dr. Bengoechea and @cggbamford
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7283846/
6/12
A nice table on #COVID_19 & #AntimicrobialResistance epidemics in CID @IDSAInfo
"Understanding how COVID-19 affects AMR trends and what we can expect if these remain the same or worsen, will help us plan next steps to tackle AMR." @schunemann_mac https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7337675/
A nice table on #COVID_19 & #AntimicrobialResistance epidemics in CID @IDSAInfo
"Understanding how COVID-19 affects AMR trends and what we can expect if these remain the same or worsen, will help us plan next steps to tackle AMR." @schunemann_mac https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7337675/
7/12
Viewpoint in @NatureRevMicro on Antimicrobial use, drug-resistant infections and #Covid_19 by @TmRawson et al.
"Consideration needs to be given to the impact of the COVID-19 pandemic on individual national action plans for AMR." https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7264971/
Viewpoint in @NatureRevMicro on Antimicrobial use, drug-resistant infections and #Covid_19 by @TmRawson et al.
"Consideration needs to be given to the impact of the COVID-19 pandemic on individual national action plans for AMR." https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7264971/
8/12
In this study from Korea, of 6871 patients with COVID-19, 2419 (35.21%) and 536 (7.80%) were prescribed total antibiotics and anti-MRSA or anti-pseudomonal antibiotics.
Authors call for antibiotic stewardship. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7604125/
In this study from Korea, of 6871 patients with COVID-19, 2419 (35.21%) and 536 (7.80%) were prescribed total antibiotics and anti-MRSA or anti-pseudomonal antibiotics.
Authors call for antibiotic stewardship. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7604125/
9/12
COVID-19 pandemic and antimicrobial resistance: Another call to strengthen laboratory diagnostic capacity in Africa https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7567179/
COVID-19 pandemic and antimicrobial resistance: Another call to strengthen laboratory diagnostic capacity in Africa https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7567179/
10/12 Interesting antimicrobial stewardship study in @ICHEJournal @milnerstaub @codeblieu
After initial increase in antibiotic use in #COVID_19 patients, starting a multispecialty COVID-19 clinical guidance team resulted in abx use decreases.
@DMAronoff https://pubmed.ncbi.nlm.nih.gov/33100250/
After initial increase in antibiotic use in #COVID_19 patients, starting a multispecialty COVID-19 clinical guidance team resulted in abx use decreases.
@DMAronoff https://pubmed.ncbi.nlm.nih.gov/33100250/
11/12
Antimicrobial stewardship: a COVID casualty?
Editorial in @jhieditor
"...we must not forget that, along with the climate crisis, AMR presents an immediate and escalating threat..." https://pubmed.ncbi.nlm.nih.gov/33045312/
Antimicrobial stewardship: a COVID casualty?
Editorial in @jhieditor
"...we must not forget that, along with the climate crisis, AMR presents an immediate and escalating threat..." https://pubmed.ncbi.nlm.nih.gov/33045312/
12/12
in JAC:
Antimicrobial stewardship challenges and innovative initiatives in the acute hospital setting during the #COVID_19 pandemic
@BSACandJAC @AlidaFeTalento @colm_bergin
https://academic.oup.com/jac/advance-article/doi/10.1093/jac/dkaa400/5917783
in JAC:
Antimicrobial stewardship challenges and innovative initiatives in the acute hospital setting during the #COVID_19 pandemic
@BSACandJAC @AlidaFeTalento @colm_bergin
https://academic.oup.com/jac/advance-article/doi/10.1093/jac/dkaa400/5917783

 Read on Twitter
Read on Twitter