Thanks to all for your interest in our study! We have received a number of great questions and thought we would try to address many of them by discussing our work in a broader discussion of COVID-19 pathogenesis…
https://www.nature.com/articles/s41590-020-00828-7
(1/21)
https://www.nature.com/articles/s41590-020-00828-7
(1/21)
Why do some SARS-CoV-2 infections progress to severe COVID-19 while most people remain asymptomatic or have relatively mild symptoms during infection? One way to think about this is to borrow (in a very loose sense) the elegant “two-hit” hypothesis from cancer genetics (2/21)
This model was first developed by Alfred Knudson, Jr. and posits that more than one “hit” to the genome is required for development of some tumors.
http://www.laskerfoundation.org/awards/show/tumor-suppressor-genes-as-a-cause-of-cancer/#alfred-g-knudsonjr (3/21)
http://www.laskerfoundation.org/awards/show/tumor-suppressor-genes-as-a-cause-of-cancer/#alfred-g-knudsonjr (3/21)
With respect to COVID-19 pathogenesis, this is very likely a disease that, in most people, arises from multiple “hits”. For example, neutralizing antibodies (nAbs) are likely to be a primary mediator of protective immunity against SARS-CoV-2 (4/21)
Absence of nAbs is almost certainly a key risk factor for disease progression. Yet not all people who progress to severe COVID-19 lack neutralizing antibodies. Other “hits” can come together to cause severe COVID-19. (5/21)
An inadequate or aberrant response in B cells, T cells, innate immune signaling, cytokine-producing cells such as monocytes and macrophages are all likely to play a role in some subset of severe COVID-19 cases. (6/21)
Yet a deficit in any one of these immune compartments is unlikely to explain all or perhaps even most cases of severe COVID-19. A small glimpse of important studies that describe immune phenotypes that may contribute to some cases of severe COVID-19...:
(7/21)
(7/21)
https://www.nature.com/articles/s41586-020-2588-y
https://science.sciencemag.org/content/370/6515/eabd4570.long
https://www.nature.com/articles/s41577-020-0402-6
https://science.sciencemag.org/content/369/6508/1210.long (8/21)
https://science.sciencemag.org/content/370/6515/eabd4570.long
https://www.nature.com/articles/s41577-020-0402-6
https://science.sciencemag.org/content/369/6508/1210.long (8/21)
Additional “hits” that are clear contributors to susceptibility are comorbidities such as diabetes, cancer, obesity, smoking, heart disease:
https://www.nature.com/articles/s41591-020-0979-0
https://www.cdc.gov/coronavirus/2019-ncov/need-extra-precautions/people-with-medical-conditions.html (9/21)
https://www.nature.com/articles/s41591-020-0979-0
https://www.cdc.gov/coronavirus/2019-ncov/need-extra-precautions/people-with-medical-conditions.html (9/21)
Now to our current study…
We observed that a subset of severe COVID-19 patients produced antibody types that cause stronger activating/inflammatory cell signaling through receptors that are expressed on a variety of immune cells. (10/21)
We observed that a subset of severe COVID-19 patients produced antibody types that cause stronger activating/inflammatory cell signaling through receptors that are expressed on a variety of immune cells. (10/21)
Namely, we observed enriched production of anti-CoV2 IgG3 and IgG1 with afucosylated Fc glycoforms. Other groups are contributing similar findings (again, only a small sliver, please add to any of these lists):
https://www.medrxiv.org/content/10.1101/2020.10.07.20208603v1.full
https://journals.plos.org/plospathogens/article/file?id=10.1371/journal.ppat.1008796&type=printable
(11/21)
https://www.medrxiv.org/content/10.1101/2020.10.07.20208603v1.full
https://journals.plos.org/plospathogens/article/file?id=10.1371/journal.ppat.1008796&type=printable
(11/21)
https://www.biorxiv.org/content/biorxiv/early/2020/05/18/2020.05.18.099507.full.pdf
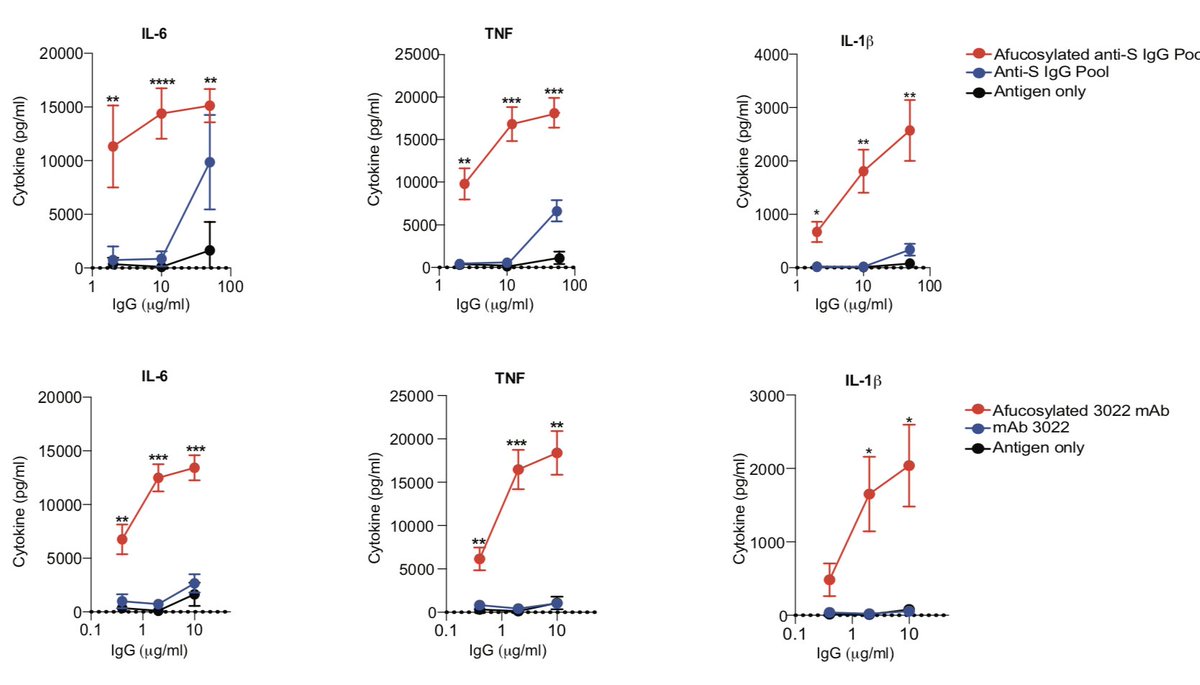
One readout for the activity of afucosylated anti-CoV2 IgG1 is enhanced production of inflammatory cytokines after incubation of CoV2 immune complexes with primary monocytes (12/21).
One readout for the activity of afucosylated anti-CoV2 IgG1 is enhanced production of inflammatory cytokines after incubation of CoV2 immune complexes with primary monocytes (12/21).
Some of these cytokines have been associated with a subset of severe COVID-19 cases.
https://www.nature.com/articles/s41591-020-1051-9 (13/21)
https://www.nature.com/articles/s41591-020-1051-9 (13/21)
The presence of these antibodies and associated immune complexes may be one “hit” that tips the balance towards a deleterious amount of inflammation, promoting disease progression in a subset of severe COVID-19 cases. (14/21)
Alternatively, these antibody Fc structures may not be involved in pathogenesis at all -they may simply be a marker of higher risk. Much more work is needed to understand this.(15/21)
Interestingly, production of afucosylated IgG1 is also observed in some severe dengue virus infections:
https://science.sciencemag.org/content/355/6323/395.long (16/21)
https://science.sciencemag.org/content/355/6323/395.long (16/21)
Production of these more highly inflammatory antibody forms may be a response to some severe viral infections; they may also be an antecedent to infection in some cases.
(17/21)
(17/21)
A couple of important points:
Our study does not suggest that anti-CoV-2 nAbs for therapeutic use should be “null” for Fc gamma receptor binding. On the contrary, Fc engineering to promote interactions with specific activating FcγRs may well be a useful strategy... (18/21)
Our study does not suggest that anti-CoV-2 nAbs for therapeutic use should be “null” for Fc gamma receptor binding. On the contrary, Fc engineering to promote interactions with specific activating FcγRs may well be a useful strategy... (18/21)
...to enhance protection by therapeutic CoV2 mAbs. A very interesting first demonstration of this here:
https://www.biorxiv.org/content/10.1101/2020.09.15.298067v1.full (19/21)
https://www.biorxiv.org/content/10.1101/2020.09.15.298067v1.full (19/21)
Finally, this study definitely does not suggest that vaccination against SARS-CoV-2 may be dangerous. Effective vaccines work by eliciting protective immunity that negates the impact of pre-existing “hits” that may cause an individual to be at risk during infection. (20/21)
The emerging data from SARS-CoV-2 vaccine studies are extremely encouraging and we eagerly await the opportunity to be vaccinated against this virus. (21/21)

 Read on Twitter
Read on Twitter