1/My latest:"What Makes a Prescriber Stop Opioid Prescriptions if they Believe it Could Harm the Patient? Let’s Talk About Metrics and Systems" -tries to reduce confusion about how US health systems misconstrue the 2016 @CDCgov #opioid Guideline- https://medium.com/@StefanKertesz/what-makes-a-prescriber-stop-opioid-prescriptions-if-they-believe-it-could-harm-the-patient-2bb4ce5d19db
2/The focus is NOT whether opioid taper can be good. It can be. I'm focused on another thing: how US-based clinicians decide they *must* do it *even when they believe it could harm the patient*. It comes down to specific policy levers across US health-care.
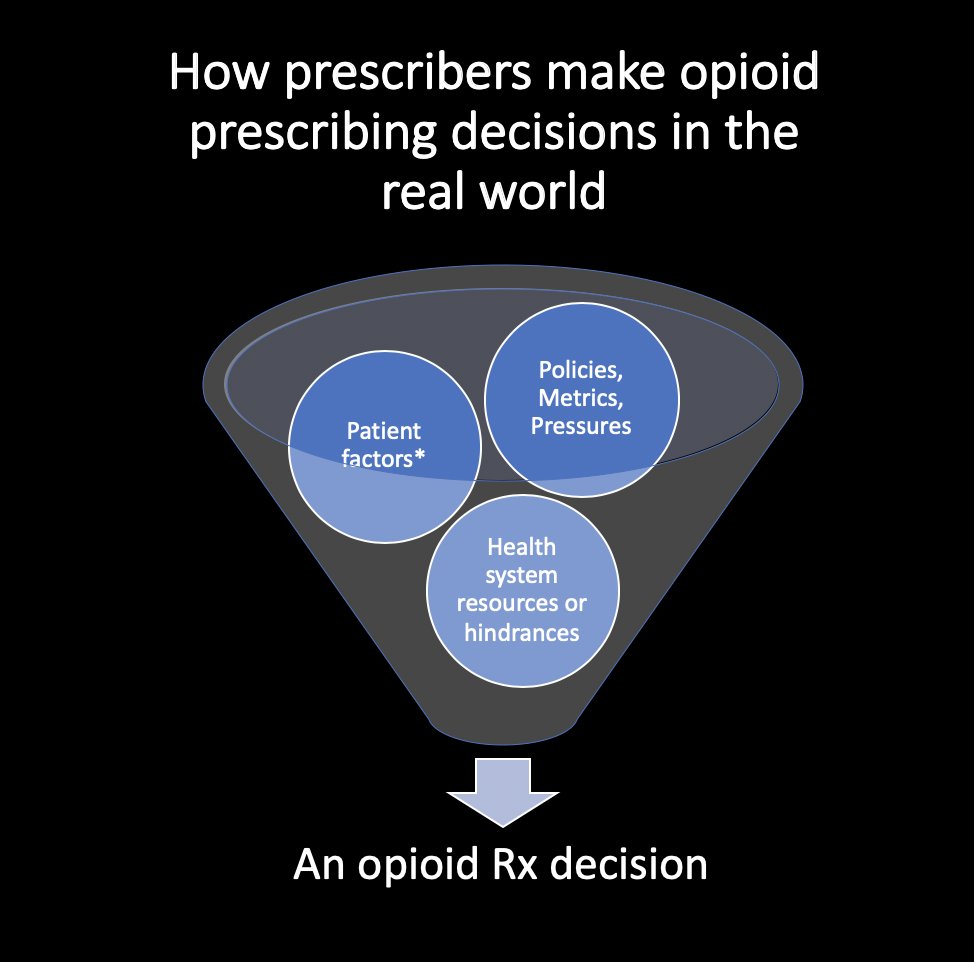
3/It's never "just one thing". It's not just insurance, or just metrics, or just emotion. A bucket of factors feed in. But this new piece focuses on "Polices, Metrics, Pressures" in particular. I want to credit @tal7291 for helping me think this through
4/And one more cautionary: the core problem is not our metrics & our systems It's that most of us clinicians, and our training programs, and our health systems, fail to inculcate an understanding of:
Pain care
Rehabilitation
Dependence or addiction
Pain care
Rehabilitation
Dependence or addiction
5/But, in the context of crappy education for pain, rehabilitation or care of dependence, or addiction, we have set up systems for care management that screw up care. Both governmental and nongovernmental agencies contribute. https://medium.com/@StefanKertesz/what-makes-a-prescriber-stop-opioid-prescriptions-if-they-believe-it-could-harm-the-patient-2bb4ce5d19db

 Read on Twitter
Read on Twitter